Why are tests used to measure breathing during sleep?
Your doctor may test you for sleep disordered breathing (SDB) if you have some or all these symptoms:
- waking feeling unrefreshed
- feeling tired in the day
- morning headaches
- loud snoring
- gasping, snorting or choking at night
- disturbed sleep
- low oxygen levels
- high carbon dioxide levels
- breathing that stops and starts.
You may need one or more sleep tests if you have these symptoms. Talk to your GP if you have these symptoms and they can refer you to a specialist clinic for tests.
Preparing for your sleep tests
You will have a first appointment at a local sleep centre or hospital. You will meet with a sleep consultant who may ask you about:
- your symptoms
- how long you have been affected
- any medications you take – sleeping tablets, anti-depressants and prescribed painkillers can affect your sleep and make you more tired in the day.
They will also ask you to complete a sleep questionnaire about how sleepy you are in the daytime. You may be offered a sleep study at home or in a clinic.
Before your sleep tests
Before your sleep study, you should:
- avoid alcohol and caffeine on the day of your test - alcohol and caffeine can affect your sleep and make some sleeping disorders worse
- try to avoid sleeping during the daytime
- avoid using creams, hair gel, make-up, or nail varnish before the test - these can affect the way the test works
- continue to take any regular medications as normal
Types of sleep test
Respiratory polygraphy sleep test
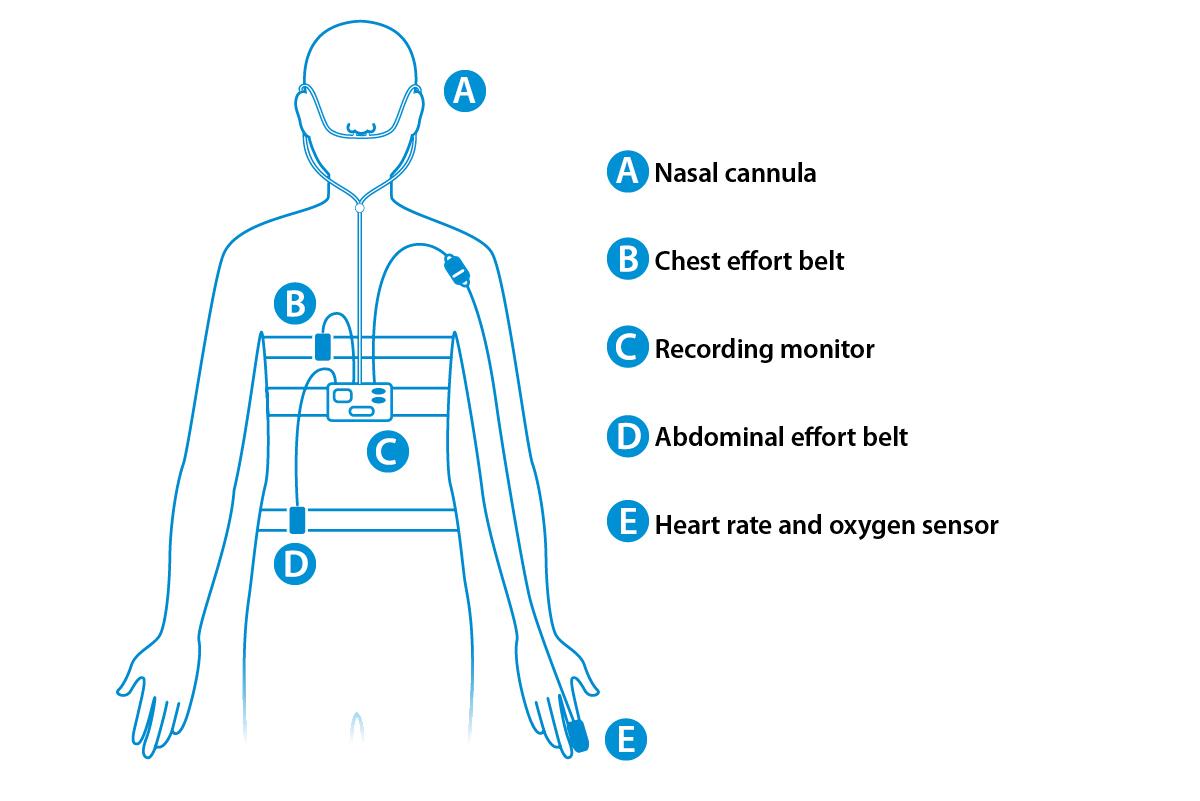
A respiratory polygraphy sleep test is used to diagnose sleep disordered breathing (SDB), which can include conditions such as obstructive sleep apnoea (OSA). Most people can do this test at home.
You’ll wear some equipment while you sleep to record your:
- breathing
- oxygen levels
- heart rate
- snoring
- sleep position and movement.
Recording oxygen and carbon dioxide levels overnight
Sometimes, your doctor may want to monitor your oxygen levels overnight. You’ll do a test called overnight oximetry. This may be used to diagnose a condition or to ensure your current treatment is effective.
You wear a small clip on your finger, or sometimes on your earlobe, known as a pulse oximeter. This can record your oxygen levels and your heart rate overnight.
In some people, doctors may also want to know your carbon dioxide (CO2) levels. They may do a blood test from your ear or your wrist. Some centres may use a transcutaneous CO2 monitor. This uses an electrode, usually on your ear, to record CO2 levels through the skin.
Polysomnography (PSG)
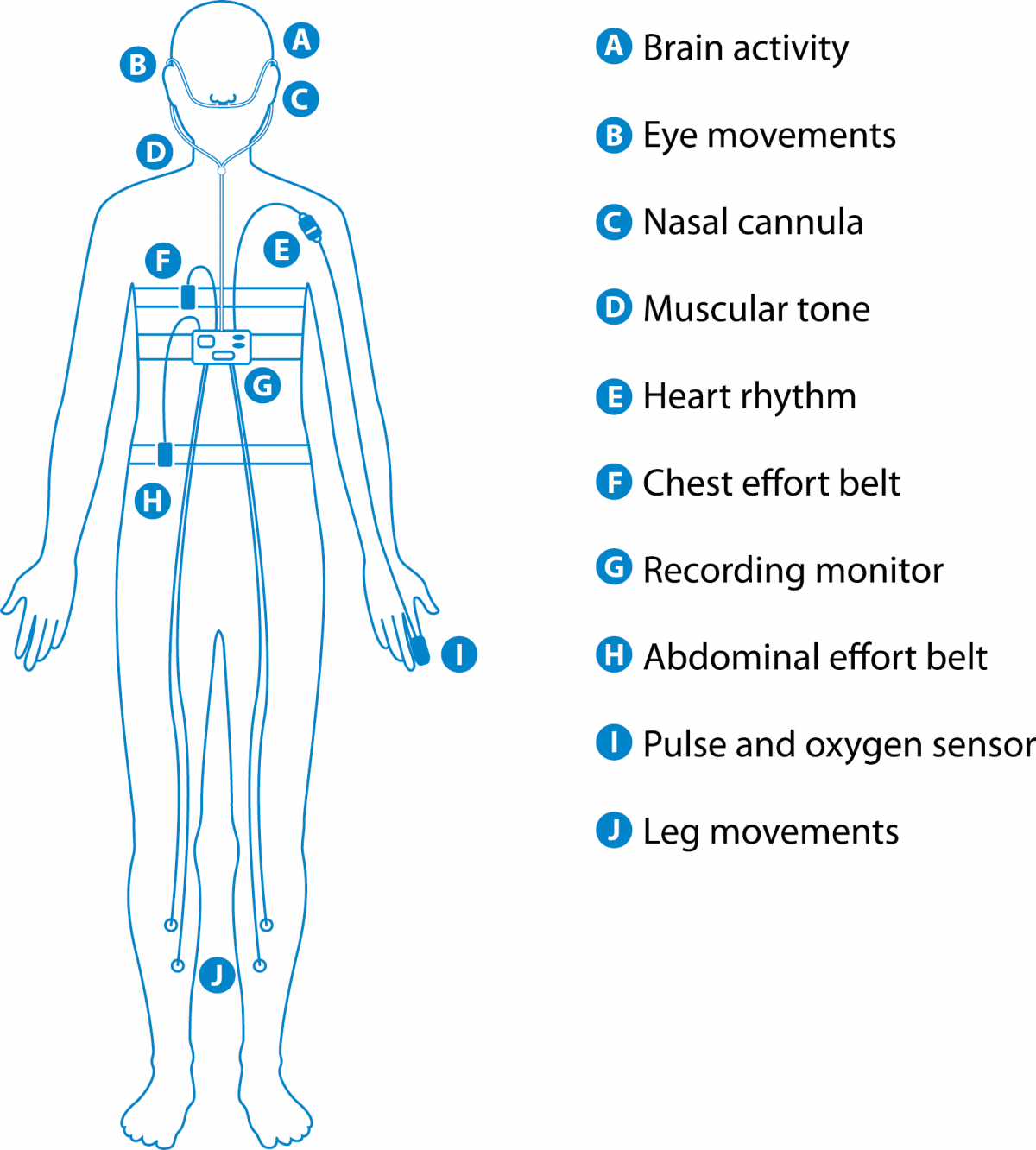
PSG is a test used to study the changes that happen when you sleep. It’s an overnight study in a quiet hospital room. It’s designed to assess:
- brain activity
- eye movements
- muscle activity
- heart rhythm
- breathing signals (air flow, chest movement)
- oxygen levels.
PSG is used to rule out many types of sleep disorders, including obstructive sleep apnoea (OSA).
Multiple sleep latency test
Your sleep specialist may ask you to stay in hospital after the overnight stay for a multiple sleep latency test. You’ll be asked to nap for 20 minutes at set times. You keep on the same equipment you had for the polysomnography.
Maintenance of wakefulness test
The specialist may want to know how alert you are during the day and how easily you fall asleep. You’ll do a maintenance of wakefulness test during the day, following your overnight stay.
You’ll be asked to stay awake for as long as you can, sitting still in a quiet, relaxing, semi-darkened room. You’ll keep on the same equipment you had for the polysomnography.
OSLER test
An Oxford sleep resistance (OSLER) test measures the amount of time you can stay awake in conditions that are comfortable to fall asleep. This test is performed during the daytime.
You will be asked to lie in an upright position in a quiet, darkened room. You will have a handheld box with a button to press every time you see a red light.

Get support
Call or email our helpline for support with any aspect of living with asthma – whether you need practical advice, emotional support, or answers to health-related questions. You can also find support through our groups.
This content is currently being reviewed. Updated information will be available soon.








