Types of breathlessness
Getting out of breath is normal. It’s a natural response when your body needs more oxygen and energy after doing something physical. For example, when you run for a bus.
Some people get out of breath even when they’re not being active. They suddenly find it difficult or uncomfortable to breathe and may feel they can’t control their breathing.
In the UK, 1 in 10 people experience breathlessness. And 1 in 5 people who visit A&E are there because of breathlessness.
Chronic breathlessness
Chronic means long-term. Chronic breathlessness develops gradually and can last for weeks, months, or years. Sometimes people also cough, bring up phlegm or feel wheezy.
Acute breathlessness
Acute means getting suddenly and unexpectedly out of breath. Acute breathlessness needs to be tested or treated straight away as it can be a sign of a new medical condition.
Call 999 or go to A&E if:
You have sudden shortness of breath and:
- your chest feels tight and heavy
- you have pain spreading to your arms, back, neck or jaw
- you feel sick or are being sick
- you’re coughing up blood
- you have pain or swelling in one of your legs.
How breathlessness feels
Breathlessness is not just physical. It’s also a feeling that affects the way we think and act. We each feel it differently.
- You may feel hot, panicky or overwhelmed.
- Your chest might feel so tight, it feels like you can’t breathe in properly.
- You might feel you’re suffocating, and you need to take deep breaths but can’t.
- You might feel breathing is very hard work and exhausting.
Breathlessness and worry
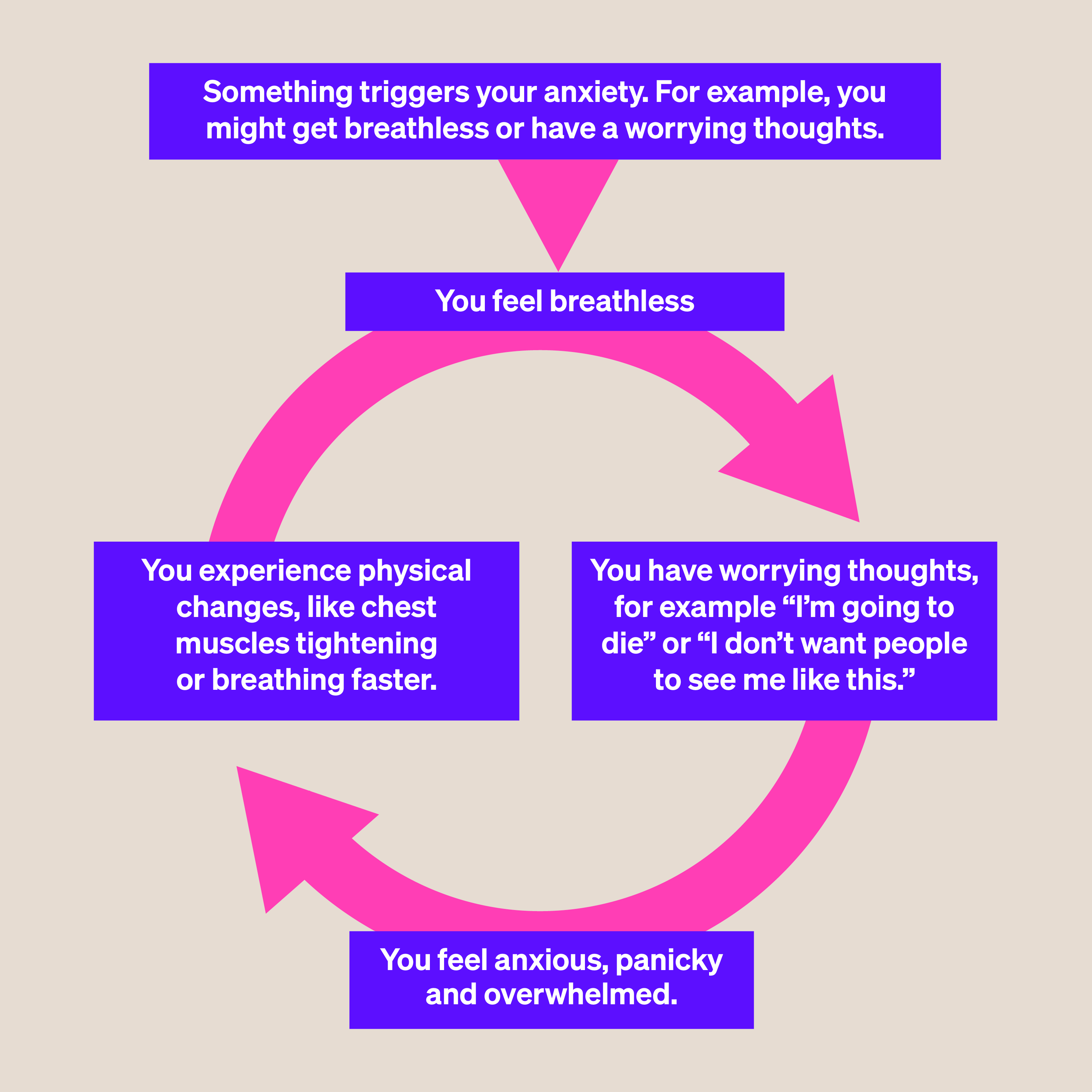
Getting out of breath can be frightening and make you feel anxious. That anxiety or worry can increase how breathless you feel. As we get more anxious, we may become more aware of our breathing, breathe faster, and tense our breathing muscles. This can lead to a panic attack.
Causes of breathlessness
If you’re feeling breathless when you wouldn’t normally be, you should see your GP straight away. The most common causes of breathlessness are:
- lung conditions like COPD (chronic obstructive pulmonary disease)
- heart conditions
- anxiety
- being overweight
- smoking.
Other causes of breathlessness can be:
- allergic reactions (anaphylaxis)
- anaemia
- complications of diabetes (diabetic ketoacidosis).
Diagnosing breathlessness
There are a number of breathing tests and lung function tests your GP may refer you for if you’re experiencing breathlessness.
Firstly, you’re likely to have an assessment so that your GP or healthcare professional knows:
- your medical history
- smoking history
- body mass index (BMI).
You may then have further tests like:
- electrocardiogram (ECG)
- Chest X-rays
- Spirometry
- FeNO (Fractional Exhaled Nitric Oxide)
- MRC (Medical Research Council) Breathlessness Scale.
The MRC Breathlessness Scale
The tool healthcare professionals usually use to measure breathlessness is the Medical Research Council (MRC) breathlessness scale. This does not recognise other aspects of breathlessness – such as how you think or feel about getting out of breath.
The MRC scale shows what your breathlessness stops you doing. Your grade is the one that describes you when you’re at your best. Your doctor should show you the MRC breathlessness scale to help describe how breathless you get.
| Description | Grade |
| I only get breathless with strenuous exercise | 0 |
| I get short of breath when hurrying on level ground or walking up a slight hill | 1 |
| On level ground, I walk slow than people of my age because of breathlessness, or I have to stop for breath when walking at my own pace on the level | 2 |
| I stop for breath after walking about 100 yards or after a few minutes on level ground | 3 |
| I am too breathless to leave the house, or I am breathless when dressing and undressing | 4 |
Treating breathlessness
Treatment will depend on what condition you’re diagnosed with and the cause of your breathlessness. You may be prescribed medicines, or you may be referred for services like pulmonary rehabilitation to help improve your breathing muscle strength.
Support for breathlessness
Getting out of breath can be very frightening. You may feel anxious about it or feel embarrassed that other people might notice. The good news is that you can get help. Your healthcare professional will help you to manage your breathlessness.
It’s good to talk to other people about your fears and worries. Your friends and family can help to support you by understanding more about what you’re going through.
Find out more:
- How to manage your breathlessness using breathing techniques.
- Take our breath test to help you understand your breathlessness.
- Find out how to manage anxiety and depression if you have a lung condition.
- Join a support group, such as our Breathe Easy Programme.

Get support
Call or email our helpline for support with any aspect of living with a lung condition – whether you need practical advice, emotional support, or answers to health-related questions. You can also find support through our groups.








